Maria C. Katapodi, Ph.D., MSc, BSN, University of Michigan School of Nursing, Ann Arbor, MI, Noreen, C. Facione, Ph.D., FAAN, RN, University of California San Francisco, School of Nursing, San Francisco, CA, and Penny F. Pierce, PhD, RN, University of Michigan, Ann Arbor, MI.
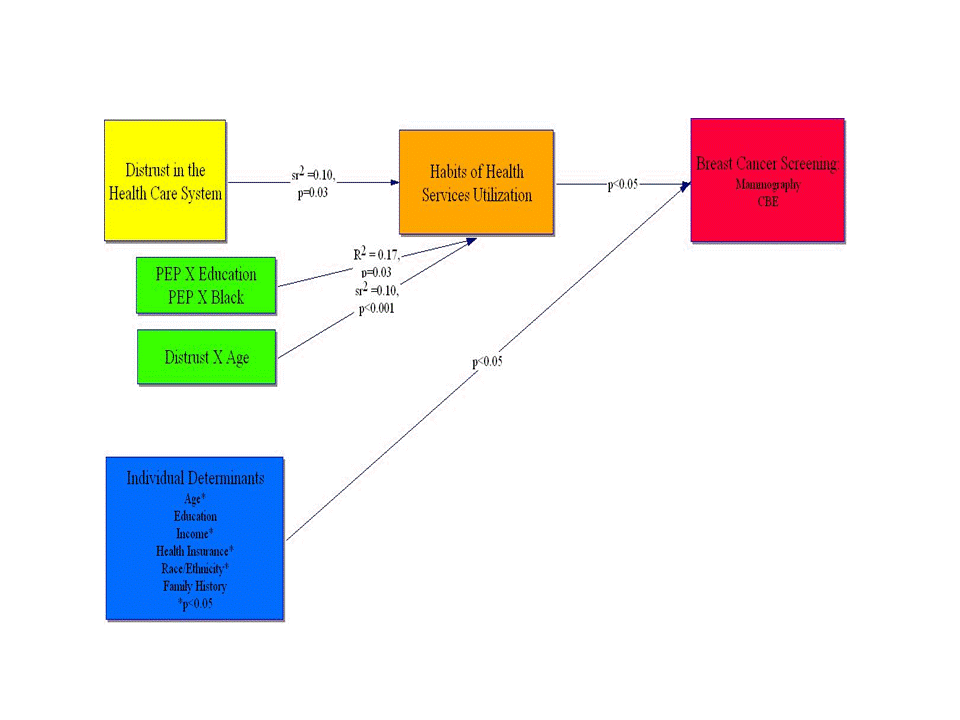
Background: Trust is based on the “asymmetry principle”, which in turn stems from cognitive biases, such as “negativity” and “confirmatory” biases. People pay more attention to trust-destroying than to trust-building information (negativity bias), and discount evidence that contradicts their own views, while they select information that supports their existing beliefs (confirmatory bias). Distrust in the health care system might influence decision-making regarding routine medical care, such as breast cancer screening. It has been attributed to cultural and ethnic differences, while less attention has been given to contributing cognitive processes. The study examined 1) the influence of distrust on predisposition to use health care services and 2) the influence of attitudinal and habitual characteristics on breast cancer screening. Methods: We recruited 184 women (age 47±12) from community settings. Most (49%) were college educated, 22% had income <$0,000/year, 77% had health insurance, and 57% were minority (27% non-Hispanic Black, 14% Hispanic, 16% Asian). Four items captured Distrust to the Health System and the negativity and confirmatory biases. Items loaded on a single principal component and explained 54% of the variance in distrust. Individual loadings ranged from 0.632 to 0.780 and Cronbach alpha=0.71. The Personally Experienced Prejudice scale measured women's personal experience of prejudice within the health system and the Habit of Health Services Utilization scale measured predisposition to use health services (Cronbach alpha=0.79 & 0.84, respectively). Results: Distrust was the single most important predictor of predisposition to use health services, which in turn was a significant predictor of breast cancer screening. Observed interactions among distrust, perceived prejudice, age, education, and race highlight the importance of distinguishing among racial/cultural, socioeconomic, and cognitive contributors to distrust. Conclusions: Distrust takes the greatest toll among vulnerable groups of women in predisposition to use health services and decision-making regarding breast cancer risk management.
See more of Poster Session IV
See more of The 28th Annual Meeting of the Society for Medical Decision Making (October 15-18, 2006)

